Managing diabetes requires consistent attention to overall health, and dental care for diabetic patient is a critical part of that routine. High blood sugar levels directly affect the gums, teeth, and oral tissues, increasing the risk of infection, inflammation, and delayed healing. Understanding how diabetes influences oral health allows patients to prevent complications and maintain long term stability.
If you are searching for the phrase dental clinic near me, one of the best clinics we recommend is Willow Dental Care Vancouver, which provides professional dental services using modern technology to ensure a comfortable and high quality experience. Professional supervision plays an essential role in dental care for diabetic patient, especially when blood glucose control fluctuates.
Why Dental Care for Diabetic Patient Is Essential
Diabetes impacts the body’s ability to fight bacteria. Since the mouth naturally contains bacteria, uncontrolled blood sugar can lead to:
- Increased plaque accumulation
- Higher risk of gum disease
- Slower healing after dental procedures
- Greater likelihood of dry mouth
- Increased risk of oral infections
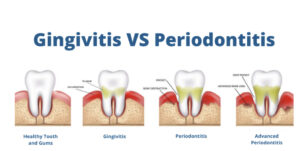
When blood glucose levels remain elevated, gum tissues become more vulnerable to inflammation. This can progress from gingivitis to periodontitis if not properly managed. Effective dental care for diabetic patient reduces these risks and supports overall metabolic stability.
How Diabetes Affects Oral Health
- Reduced immune response, making infections more severe
- Thickening of blood vessels, slowing nutrient delivery to gum tissue
- Decreased saliva production, leading to dry mouth
- Higher sugar levels in saliva, encouraging bacterial growth
Because of these factors, dental care for diabetic patient must be preventive, structured, and continuous.
Common Oral Problems in Diabetic Patients
Understanding potential complications helps patients take proactive steps.
1. Gum Disease
Periodontal disease is more common and often more severe in diabetic individuals. Symptoms include:
- Red or swollen gums
- Bleeding during brushing
- Persistent bad breath
- Gum recession
Proper dental care for diabetic patient significantly lowers the progression of periodontal disease.
2. Dry Mouth
Reduced saliva flow increases the risk of cavities and discomfort. Saliva protects enamel and controls bacteria. Without sufficient moisture, decay develops more easily.
3. Delayed Healing
After tooth extraction or gum treatment, healing may take longer. Maintaining stable blood sugar levels before procedures is essential for safe dental care for diabetic patient.
Daily Dental Care for Diabetic Patient
Consistent at home care is the foundation of oral health management.
Brushing
- Brush at least twice daily using fluoride toothpaste
- Use a soft bristled toothbrush to avoid gum irritation
- Replace toothbrush every three months
Flossing
- Floss daily to remove plaque between teeth
- Consider water flossers if manual flossing is difficult
Blood Sugar Monitoring
Maintaining stable glucose levels directly reduces oral complications. Dental care for diabetic patient begins with metabolic control.
Hydration
Drink adequate water throughout the day to reduce dry mouth symptoms and flush bacteria.
Professional Dental Care for Diabetic Patient
Regular dental visits are essential. Inform your dentist about:
- Type of diabetes
- Current medications
- HbA1c levels
- Any recent changes in health
Dentists may schedule shorter morning appointments when blood sugar is more stable. Preventive cleanings and early intervention reduce the need for invasive procedures.
Frequency of Dental Visits
- Every 6 months for well controlled diabetes
- Every 3 to 4 months if gum disease is present
Professional cleanings remove plaque buildup that cannot be eliminated at home, which is a key part of dental care for diabetic patient.
Preventive Strategies for Long Term Protection
- Maintain HbA1c within recommended range
- Avoid smoking, which increases gum disease risk
- Follow a balanced diet low in refined sugars
- Use antimicrobial mouthwash if recommended by a dentist
- Seek early treatment for gum inflammation
The relationship between diabetes and oral health is bidirectional. Poor oral health can worsen glycemic control, and unstable blood sugar can intensify gum disease. Therefore, dental care for diabetic patient supports overall health stability.
Signs That Require Immediate Attention
Diabetic patients should contact a dentist if they experience:
- Persistent gum bleeding
- Swelling or pus around gums
- Loose teeth
- Severe dry mouth
- Oral pain that does not improve
Early treatment prevents complications and supports systemic health.
The Connection Between Periodontal Health and Diabetes Control
Research shows that treating gum disease may improve blood sugar management. Inflammation from periodontal infection can interfere with insulin effectiveness. By prioritizing dental care for diabetic patient, individuals may improve both oral and systemic outcomes.
Customized Treatment Planning
Each diabetic patient requires individualized care. Factors influencing treatment planning include:
- Type and duration of diabetes
- Level of glycemic control
- Presence of cardiovascular complications
- Medication regimen
Dentists often coordinate with primary care physicians to ensure safe procedures and optimal recovery. This interdisciplinary approach enhances dental care for diabetic patient and minimizes risk.
Conclusion
Dental care for diabetic patient is not optional; it is a critical component of comprehensive diabetes management. By maintaining strict oral hygiene, attending regular dental checkups, and controlling blood sugar levels, patients can significantly reduce the risk of gum disease, infection, and delayed healing.
A proactive strategy that combines daily home care with professional supervision ensures long term oral stability and supports overall metabolic health. Consistency, awareness, and preventive care remain the most effective tools in protecting both your smile and your systemic wellbeing.